
What You Need To Know About Lung Cancer
Lung cancer and screening
Lung cancer is the second leading cause of death and the leading cause of cancer death in Thailand. Most lung cancers are diagnosed in the late stages of the disease, making treatment more problematic and as a result significantly reducing the overall lung cancer survival rate. In the past, lung cancer screening is done by chest x-ray and sputum cytology. However, these screening methods did not improve overall survival of lung cancer patients, as small nodules (subsolid nodule/ground glass nodule) cannot be detected.
In 2011, National Lung Screening Trial (NLST) in USA shows that using low dose CT-chest is an effective screening method in people who have high risk for lung cancer comparing with chest x-ray. By having once a year screening, the mortality is reduced by 20%. Therefore, currently National Comprehensive Cancer Network (NCCN), American Society of Clinical Oncology (ASCO), and American College of Chest Physicians (ACCP) recommend lung cancer screening in high risk population by using low dose CT-chest.

The high risk group is defined as:
- Age 55 – 80 years
- Current or former smokers
You may consider lung cancer screening if you have a history of smoking for 30 pack years or longer. Pack years are calculated by multiplying the number of packs of cigarettes smoked a day and the number of years that you smoked.- Smoked two packs a day for 15 years
- Smoked one pack a day for 30 years
- Smoked one and a half pack a day for 20 years
- Stop smoking less than 15 years
There are other risk factors as below:
- Age
- Sex
- Ethnicity
- Weight and height
- Education
- Family history of lung cancer, those with chronic obstructive pulmonary disease (COPD), those with other cancers
Moderate risk group
People who are in moderate risk group are current or former smokers with a history of smoking for 20 pack years, second hand smoker, or live in bad environment. Screening is not currently recommended.
Other risk factors

Incense
Research in China suggests that long-term exposure to burning incense does present a danger to the respiratory tract and this can lead to lung cancer. Therefore, people who have risks of lung cancer (family history of lung cancer, COPD, asthma) should avoid exposing to incense smoke.

Fine particular matter (PM2.5)
The term fine particles, or particulate matter 2.5 (PM2.5), refers to tiny particles or droplets in the air that are two and one half microns or less in width. Fine particles primarily come from car exhausts, operations that involve the burning of fuels such as wood, heating oil or coal, and construction. Air Quality Index (AQI) is an index for reporting air quality. AQI measures air pollutants including PM2.5. Particles in the PM2.5 size range are able to travel deeply into the respiratory tract, reaching the lungs. Exposure to fine particles can cause short-term health effects such as eye, nose, throat and lung irritation, coughing, sneezing, runny nose and shortness of breath. Exposure to fine particles can also affect lung function and worsen medical conditions such as asthma and heart disease. Moreover, the risk of developing lung cancer increases as the level of PM2.5 in the air increases. When outdoor levels of PM2.5 are elevated, it is best to avoid going outdoors, use an air purifier, and wear face mask.
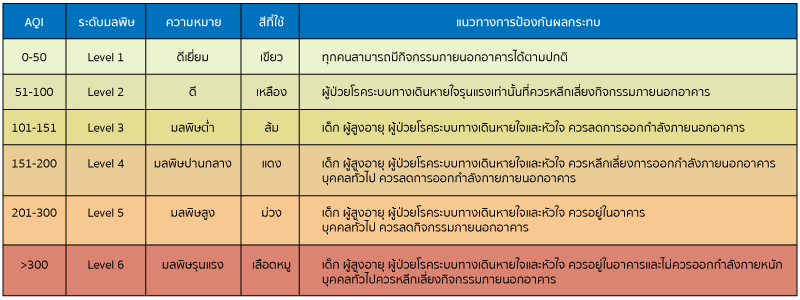
source : http://aqicn.org/city/bangkok/

E-Cigarettes
An electronic cigarette is a battery-operated device that emits doses of vaporized nicotine, or non-nicotine solutions, for the user to inhale. It can resemble traditional tobacco cigarettes, without the smoke. E-cigarette reduces the exposure to arsenic, lead, and other harmful substances in traditional cigarettes. However, that does not mean electronic cigarettes are safe. Further research will need to be completed before electronic cigarettes can be either labeled harmful or safe, while we know very well the effects of traditional cigarettes on our health. Consumers should be aware that information regarding electronic cigarettes is still preliminary. Additional research will help understand long term health effects of electronic cigarettes.

Finding lung cancer early, when it is easiest to treat, can save lives.
American Cancer Society recommends that people who are current or former smoker more than 30 pack year or stop smoking less than 15 years, and are 55 years or older should be screened for lung cancer by using low dose CT-chest once a year.
“When detected early, lung cancer patients have more treatment options and a far greater chance of survival and quality of life.”
Link: “Wattanosoth Early detection Center” Wattanosoth Early detection Center

Reference :
Dr. Padungkiat Tangpiroontham, a cardiothoracic surgeon specialized in minimally invasive thoracic surgery.
- Reduced Lung-Cancer Mortality with Low-Dose Computed Tomographic Screening. N Engl J Med 2011;365:395-409
- Evaluation of the Lung Cancer Risks at Which to Screen Ever- and Never-Smokers: Screening Rules Applied to the PLCO and NLST Cohorts.PLOS MED 2014;11:1-13
- Environ Toxicol. 2017 Nov;32(11):2379-2391. doi: 10.1002/tox.22451. Epub 2017 Jul 19.
- Rev Environ Health. 2016 Mar;31(1):155-8. doi: 10.1515/reveh-2015-0060.
- Environ Health Perspect. 2011 Nov;119(11):1641-6. doi: 10.1289/ehp.1002790.
- Environ Health Perspect. 2010 Sep;118(9):1257-60. doi: 10.1289/ehp.0901587. Epub 2010 May 14.
- Cancer. 2008 Oct 1;113(7):1676-84. doi: 10.1002/cncr.23788.
- BMJ Open. 2015 Nov 24;5(11):e009452. doi: 10.1136/bmjopen-2015-009452.
- Am J Respir Crit Care Med. 2011 Dec 15;184(12):1374-81. doi: 10.1164/rccm.201106-1011OC. Epub 2011 Oct 6
- Environ Res. 2018 Jul;164:585-596. doi: 10.1016/j.envres.2018.03.034. Epub 2018 Apr 4.
- Cancer Epidemiol Biomarkers Prev. 2017 Aug;26(8):1175-1191. doi: 10.1158/1055-9965.EPI-17-0358
- Proc Natl Acad Sci U S A. 2018 Feb 13;115(7):E1560-E1569. doi: 10.1073/pnas.1718185115
- Nicotine Tob Res. 2018 Apr 16. doi: 10.1093/ntr/nty076